Hope, Health & Healing

Hope, Health & Healing
February 10, 2022Every big idea contains a multitude of moving parts. Pieces that no single person can reign over alone. While an original idea may stem from one brain, history’s greatest innovators seldom worked solo. Because building an idea into practice is a team effort. For Michigan State University, it’s second nature to join forces with the people who can help assemble those moving parts into a single unit, working together to serve the greater good.
This is particularly true for medical education at MSU, which, for more than 70 years, has been treating the state as its campus, taking teaching and care efforts where they are needed most. It’s a reflection of the university’s land-grant philosophy. It’s also a unique stance in health care education and research. Rather than concentrating these efforts on a single site, Spartans reach out to populations in every part of Michigan. In urban cores, rural expanses and everywhere in between, MSU’s health care partnerships and community collaboration have been essential to the growth of students, the development of ideas, the health of the public and the advancement of opportunity. When everyone brings what they have to the table, big ideas become big realities. The latest example is a first-of-its-kind venture and new addition to the College of Human Medicine and the MSU Grand Rapids Innovation Park.
Take one look at the Doug Meijer Medical Innovation Building (DMMIB) and you know it’s something special. The contemporary design, featuring ribbons of windows and an impressive atrium, alludes to the big thinking happening inside. And more. There’s big collaboration that helps big ideas find their way out to effect change and progress through real-world care and solutions.
Outside, a set of larger-than-life white beams intersect and reach skyward to support the facility above, as if to represent the convergence of disciplines working and healing together under the same roof. Inside, the concept of public-private partnership takes flight, closely coupling MSU’s world-class research with private industry partners who have the talent and track record for delivering discoveries to the masses. This is where research meets outreach. Where a hunger for change and an entrepreneurial spirit work together. Where breakthroughs can and will breakthrough in the form of accessible care for all.
Even the project itself took a special kind of cooperation to complete. In 2019, MSU joined forces with Health Innovation Partners. This alliance with the real estate joint venture marked MSU’s first public-private partnership in the form of a long-term ground lease. That is, Michigan State owns the land, and Health Innovation Partners took charge of planning, construction and development.
The 200,000-square-foot space will house health research and outreach efforts ranging from cancer treatment to brain health research to medical device development. It will be home to researchers from MSU and private companies. This public-private partnership is a bold move for MSU and the health care community at large. The big idea: to inspire a health science revolution.
EXPANDING THE FOOTPRINT
Essential to understanding the role of this new facility is understanding MSU’s existing health partnerships in Grand Rapids. Home to the College of Human Medicine, the privately funded Secchia Center opened in 2010 and provides world-class medical education. Seven years later, the Grand Rapids Research Center opened its doors and currently houses 33 research teams seeking modern solutions in areas such as Alzheimer’s disease, Parkinson’s disease, autism and women’s health. So, with well-established medical education and biomedical research, MSU moved to fill in the final blank with the DMMIB.
“Once you discover something and translate it back down to care, how do people get access to that care? The way you get access is to bring in industry partners, side by side, so that the things you discover can get taken to people where they live,” Executive Vice President for Health Sciences Norman J. Beauchamp Jr., M.D., says of innovative treatments and medical developments. “Because one of the challenges in health care is you often have to know someone who knows someone to get access.”
That’s what makes this piece so pivotal. MSU working alongside private companies in the same facility allows a free exchange of ideas and resources. It gives discoveries a clearer path to distribution, which leads to easier public access to care. The work is already underway with Bold Advance Medical Future Health, which specializes in nuclear theranostics, a process that uses a combination of radioactive drugs to diagnose and eliminate tumors with extreme precision. The team’s work, led by Dr. Anthony Chang, is bolstered by MSU’s two new cyclotrons, bringing the world’s most advanced radiopharmacy to West Michigan. Until now, this lifesaving technology, which delivers the most effective, efficient, non-invasive diagnostics and treatments for cancers and neurogenerative diseases available to date, wasn’t available in North America.
Also taking up residence in the MSU Grand Rapids Innovation Park will be Perrigo Company plc. The pharmaceutical company broke ground on its North American corporate headquarters in April 2021 and shares MSU’s vision of treating people as close to home as possible.
But it’s not just large enterprises moving in. The DMMIB is also creating innovation space for startups and entrepreneurial high-tech companies. Over the past decade, the innovation landscape has shifted. Large companies are spending less time and money innovating in-house. Instead, they wait for startups to innovate, build and grow before acquiring the fledgling companies. MSU identified an opportunity to foster entrepreneurship in the facility.
“Once you discover something and translate it back down to care, how do people get access to that care? The way you get access is to bring in industry partners, side by side, so that the things you discover can get taken to people where they live.”
— NORMAN J. BEAUCHAMP JR., M.D.
Executive Vice President for Health Sciences at Michigan State University
“Here, the goal is to help startups grow to a point where they can partner with large companies,” says Frank Urban, director of venture creation at Spartan Innovations, which will have a presence in the DMMIB. The group will also manage Grand Rapids’ SmartZone Business Incubator alongside local seed accelerator Smart Garden. “As we build that, you’ll see other companies and larger corporations become attracted to the area, bring jobs to the area and create opportunity well into the future.”
As a subsidiary of the MSU Foundation, Spartan Innovations drives MSU entrepreneurs to develop their ideas and launch high-tech startups. Moving in alongside Spartan Innovations is another MSU Foundation offshoot, Red Cedar Ventures, which has been helping accelerate the commercialization of startups since 2014.
With investors, accounting groups, contract research and contract manufacturing organizations outside their doors, young companies will have full access to a wealth of services and research capabilities—an unparalleled infrastructure of support for advancing ideas and making them happen.
BRINGING IT HOME
While the DMMIB opens doors for private and public researchers and innovators, it all builds back to the shared goal of MSU and every partner: reducing health disparities in communities across the state and the country.
“The whole construct of this eco-system is going from what do people need? How do we solve it? And how do we get it to people?” Beauchamp says of MSU’s involvement in West Michigan.
Doug Meijer pondered the latter question throughout the course of his medical journey. After a 2011 prostate cancer diagnosis, Meijer followed the traditional treatment path, but saw little improvement. He toured the nation’s top hospitals seeking answers before an introduction to Dr. Chang led him to Germany for a theranostics test study. The treatment saved his life with virtually no side effects. He wanted to help bring that groundbreaking technology home.
“You have to travel to Germany to get this treatment,” says Meijer. “Not only that, you have to know somebody to do it. And then you have to have the wherewithal [to travel]. We didn’t think that was right.”
Thanks to a $19.5 million gift from Doug Meijer and the Meijer Foundation, that treatment has come home in a big way.
COVERING THE STATE
With all that’s happening in Grand Rapids, Beauchamp knows there is and will be plenty to share. “The goal here is to extend to other networks via partnerships throughout the state,” he says. And MSU’s efforts aren’t limited to one region. Spartans are working to advance medicine and provide accessible health care in communities all over Michigan.
Michigan State has been entrenched in the Detroit-area health care scene for many years. A long-standing alliance between the Detroit Medical Center and the College of Osteopathic Medicine trains the next generation of doctors in specialties and subspecialties across the network’s eight hospitals. And through programs like Detroit Street Care and Spartan Street Medicine, they also offer care and support for people experiencing homelessness, taking their skills and compassion where they are needed.
Also making an impact on Detroit communities is the College of Nursing, which works in partnership with the DMC to train students in the accelerated Bachelor of Science in Nursing program. The college also works with Detroit-area organizations to help better serve people’s needs. Like the upcoming collaboration with Detroit Public Schools, which will see MSU students working with students with special needs, and a partnership with the Luke Clinic, where Spartans will help provide clinical care for expectant mothers and infants as soon as spring 2022.
In 2021, MSU announced a 30-year partnership with the Henry Ford Health System, a landmark alliance that pairs Michigan State with one of the nation’s leading integrated academic health systems.
“We don’t want to make incremental change,” says Dr. Steven Kalkanis, president of the partnership’s newly formed HFH+MSU Health Sciences. “We want to change the world.”
With an overall goal of improving clinical outcomes for all communities while contributing to the global advancement of care, the collaboration is aligned with MSU’s mission of making real, positive impact for people where they live. To achieve that, the team is embedding justice, diversity, equity and inclusion into everything they do. That includes a commitment to educate diverse health care providers to better reflect the communities they serve. It also means opening health care opportunities to underserved populations. Together, Henry Ford and MSU will help provide equitable access to care—a pillar of strong, vibrant communities.
“If we bring additional focus to traditionally marginalized communities,” says Wright L. Lassiter, president and CEO of Henry Ford Health System, “we believe that will lead to improved clinical outcomes for all.”
HFH+MSU Health Sciences integrates a network of health care providers, scientists, researchers and public health practitioners to drive clinical and academic innovation. And with a leading-edge cancer center that also combines research and clinical functions, access to innovative treatment will soon be much closer to home for thousands. It’s also another opportunity to close the gap in health care outcomes. This time for cancer patients, who are often marginalized based on race, ethnicity, gender and socioeconomic status.
“Working together, we have the ability to fast-track cancer research, screening for our populations, the development of new cures, the development of clinical trials and really be a destination for all aspects of cancer,” says Kalkanis.
When a top academic institution and a leading integrated health system join forces, they have a unique opportunity to connect top minds with top resources. MSU will welcome 115 new researchers from Henry Ford Health to the university. It’s the kind of collaboration that sparks innovation and exploration, especially when it comes to community engagement. Research programs that include underrepresented populations and clinical studies to identify intervention for disparities are already underway. There is also a regional campus in development, giving the two institutions a shared space to change the way individuals and communities experience care.
These are the types of partnership extensions Beauchamp is talking about. The research and discoveries that come from one place go on to make a difference in communities everywhere.
“It’s not just about Detroit and East Lansing,” says Kalkanis. “It’s about Grand Rapids and Jackson and Wyandotte and Macomb and all the points in between, the communities in which we serve.”
Those communities are many. In Flint, Michigan State has created a culture of community collaboration alongside a roster of partners that reach out to a large and diverse population. MSU has had a presence in Flint since 1913 and has been partnering with the people of the city for equally as long. In fall 2014, a new medical education and public health research space was unveiled in the historic Flint Journal building.
Through affiliations with Ascension Genesys, Hurley Medical Center and McLaren, MSU works with community leaders to improve health services and outcomes in Flint. Social outreach also plays a vital role in education and training, which lets students engage with the communities they serve. A better understanding of the people they’re helping leads to improved care and more positive relationships with community health partners.
“In these partnerships, all have a voice in how public health projects are planned, implemented and evaluated,” says Dr. Rodlescia Sneed, assistant professor in the Department of Family Medicine and online Master of Public Health faculty. “The work to be done is not easy—but it’s certainly rewarding.”
Flint is home to MSU’s Division of Public Health, where Spartans work community partners to address the needs of the region in community-led ways. The results have been equal parts effective and inspiring. One notable example is MSU-Hurley Children’s Hospital Pediatric Public Health Initiative’s response to the limited access to healthy food—a common disparity in underserved areas. Through the Pediatric Prescriptions Program, families are given prescriptions that can be filled in the form of fresh fruits and vegetables at the Flint Farmers’ Market. The program was such a success it was implemented nationwide as part of the 2018 U.S. Farm Bill, drafted with leadership from Michigan Sen. Debbie Stabenow.
Key to MSU’s involvement in Flint is ensuring that public health decisions are made in partnership with the community. Their voices lead the way, and this makes the city a model for community-led public health.
“We do public health with the community. Not in the community, not for the community,” says Jill Vondrasek, health care communicator for the College of Human Medicine’s Division of Public Health. “Community members are our partners and our inspiration. It is their voice that informs MSU’s public health response in Flint.”
That partnership is how social needs are met. For many in the area, transportation is a challenge. To make health care visits more accessible, MSU-Hurley Children’s Hospital and MSU’s medical education and public health research space are located across the street from Flint’s main mass transit hub. And it’s no accident that the Flint Farmers’ Market shares a parking lot with these two institutions, as it allows families to visit their doctors and fill their produce prescriptions in the same visit.
“The work we do in community engagement is really innovative,” adds Sneed. “Community members have a heart for their communities, and that’s contagious.”
That kind of real-world thinking and community partnership doesn’t end at the city limits. Rural populations face their own set of health care challenges. Compared to their urban and suburban counterparts, people in rural communities are less likely to have jobs that provide health insurance or pharmacy benefits. They often must travel great distances for care and can lack broadband internet access, making telehealth visits a challenge.
“In these partnerships, all have a voice in how public health projects are planned, implemented and evaluated. The work to be done is not easy—but it’s certainly rewarding.”
— DR. RODLESCIA SNEED
Assistant Professor, MSU Department of Family Medicine
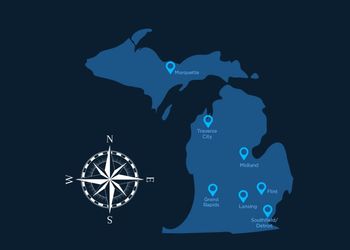
MSU’s Leadership in Rural Medicine programs prepare medical students to work in these underserved communities through partnerships with local clinics and hospitals. At campuses in Marquette, Traverse City and Midland, students spend much of their time immersed in smaller rural communities around the state. Not only as caregivers, but also as community residents.
“They don’t just go for clinical experiences, they actually live within that community while they’re there,” says Dr. Andrea Wendling, professor and director of rural health curriculum. “They have an enhanced curriculum where they work with hospital leadership, community health departments and with the public health medical director of the region.”
The program also puts students side by side with members of the community. “They learn about housing options,” Wendling continues. “They learn about educational opportunities and major employers. They visit different places within the community, so they can really understand the patient’s experience.”
Given Michigan State’s commitment to communities throughout the state, it’s no surprise that the rural medicine program was one of the nation’s first, dating back to 1975 when the inaugural class began their training at St. Francis Hospital in Escanaba. Today, Wendling says many of the students in the rural physician and rural community health programs come from rural areas: “A lot of them have seen the problems within their communities; they have had family members who are sick and they may have had gaps in care because of this disparity. They want to go back and make a difference.”
It’s another example of MSU meeting people where it matters most: close to home.
Whether public or private, academic or clinical, the health care partnerships that thrive throughout the state are consistently focused on people and communities. They have emboldened and enlivened the thinking and doing as Michigan State seeks to increase accessibility and reduce health disparities. It’s made MSU a launchpad for innovative, inclusive research and treatment. But it couldn’t be done without reaching outside our walls to shake hands with the people who could help make the moving pieces move a little better. Not for each other, but for everyone.
When it comes to these partnerships, Beauchamp sums it up best: “Together, we will transform health care and prove that hope, health and healing can be made available to all people.”
It’s a big idea. And it’s coming to life before our eyes.
Author: Tim Cerullo, '08